| • Home Page | • About Us | • TR CASE STUDY | • Program Protocol & Links |
| Charles Sourby MS Ed. |
Lehman College
THE RELATIONSHIP BETWEEN THERAPEUTIC RECREATION AND PALLIATION
IN THE TREATMENT OF THE PATIENT WHO HAS ADVANCED CANCER
Research Thesis
Charles Sourby
May 1998
CONTENTS
ACKNOWLEDGMENTS .............................................................................. ii
CHAPTER I
Introduction .................................................................................................. 3
The Problem and Purpose of the Study ........................................................... 5
Delimitation’s ................................................................................................ 6
Limitations .................................................................................................... 5
Hypotheses .................................................................................................. 7
Significance of the Study ........................................,...................................... 7
Definitions of Terms ...................................................................................... 8
. CHAPTER II
Introduction ................................................................................................ 10
Palliation .................................................................................................... 10
The Psycho-Social Impact of Dying ............................................................... 11
Role of TR .................................................................................................. .13
TR, Palliation, and the Quality of Life ........................................................ ...19
CHAPTER III ............................................................................................... 21
Research Design ........................................................................................ .21
Measures and Instruments ......................................................................... ..21
Description of the Setting ........................................................................... ..22
Subject Selection ........................................................................................ 24
Description of the Patient ........................................................................... ..26
CHAPTER IV
Results ....................................................................................................... 28
Process Notes ............................................................................................ 30
Table 1 ....................................................................................................... 43
Follow Up Interview .................................................................................... ..44
Description of the Setting ........................................................................... ..41
CHAPTER V
Conclusion ...............................................................................................47
Implications & Recommendations ............................................................... 55
REFERENCES ..........................................................................................55
CHAPTER I
INTRODUCTION
Therapeutic recreation(TR) professionals, traditionally concerned with the quality and potential of human life, face a difficult challenge in providing TR in settings that serve people with life threatening illnesses such as advanced or end-stage cancer. Despite all of the technological advances in medical treatment in the latter part of the twentieth century, some cancers quite simply cannot be cured, but treatment for pain and emotional suffering must continue(Cimino, 1997).
According to the National Cancer Institute(NCI), cancer affects people from all cultures, socio-economic classes, ages, and backgrounds (CNN, 1997). More than 1.2 million Americans are diagnosed with cancer each year and no less than 500,000 die from the disease annually (CNN, 1997). Treatment often involves surgery, radiation, and chemotherapy. The disease and subsequent treatments can be painful and uncomfortable. It is natural for anyone facing cancer to be concerned with what the future holds. Understanding the nature of cancer and what to expect can help patients and their loved ones plan treatment, anticipate lifestyle changes and make quality of life and financial decisions (OncoLink, 1997). Cancer patients frequently ask their doctor (or search on their own) for statistics to answer the question: “What is my prognosis?” (OncoLink, 1997).
Prognosis is a statistical prediction of the future course and outcome of the disease and is the likelihood of recovery (Harpham, 1994). When doctors discuss a patient’s prognosis, they are attempting to project what is likely to occur for an individual patient (Harpham, 1994). The doctor may speak of a favorable prognosis if the patient is expected to respond well to treatment, or and unfavorable prognosis if the cancer is likely to be difficult to control (Harpham, 1994).
For the patient who does not respond to treatment, or, who is medically determined to be at the end stage of the disease, being admitted to a hospital or hospice is a common occurrence. Treatment for the patient at the terminal or end stage of cancer increasingly involves an approach called palliative care.
Specifically, the palliative approach to treatment includes control of pain and other symptoms while simultaneously addressing the individual patient’s psychological, social, and spiritual concerns in an effort to achieve the best possible quality of life for the dying patient as well as his or her family (Stjernsward & Colleau, 1996). The psycho-social impact of dying is monumental, involving the search for meaning, confronting fears, dealing with the loss of control, and issues of loss (Stjernsward & Colleau, 1996).The dying patient often experiences anger, guilt, disorganization, isolation, and depression (Rando, 1984).
Therapeutic recreation contributes to the palliative treatment process by providing patients with an opportunity to gain a sense of control, develop new skills, facilitate feelings of self-satisfaction and enjoyment, as well as a means to appropriately express emotions (Willets & Sperling, 1983).
The primary role of TR is to assist patients in the development of their personal capacity to cope with the disease process and its subsequent affective symptoms such as psychological distress and depression (Willets & Sperling, 1983). Therefore, the role of TR in the treatment of advanced cancer patients is to support palliative goals.
THE PROBLEM & PURPOSE OF THE STUDY
The purpose of this study was to investigate the relationship between TR and palliation in the treatment of the patient with advanced cancer in a clinical setting. The problem was to find a causal attribution between TR and palliation; in that TR contributes to palliation by reducing or relieving symptoms of the disease, increasing appropriate functioning, and increasing a patient’s ability to cope with dying.
DELIMITATIONS
This study is delimited to one advanced cancer patient in a New York City hospital with less than six months to live. The patient was observed while participating in TR groups, at individual TR activities and at an interview about the benefits of TR. In addition, contributing information was drawn from and includes medical chart documentation and interdisciplinary team feedback.
The patient was followed from admission for one week to obtain base line data and was studied with a concentrated focus for the next two weeks as described above. This is to be a case study where the numerical identification of the subject is illustrated by the equation: (N=1).
LIMITATIONS
The average life expectancy upon admission to the hospital is less than thirty days and is determined by the fluctuating health status of the patient, the effects of medication, outside interference, and the subjectivity of the subject’s responses. Furthermore, it must be stated that a case study is generalizable to theory, not to populations (Henderson, 1991).
Uncontrolled variables are numerous because TR is conducted at bedside, in the day rooms, and in general recreation areas, where physical conditions such as the temperature, humidity, lighting, and ambient noise are out of the researcher’s control. Other uncontrolled variables include visitors who may join a TR group at any time; disruptions such as fire drills, and assorted distractions that may alter or have an unknown effect on desired outcomes.
Compromises to internal & external validity are all considered in reference to the subjective nature of the qualitative data being collected (Henderson, 1991). Every effort is made to process the data following each session with documentation, archival records, participant observation, discussion, interviews and process notes over a specific period of time(Henderson, 1991). This includes the in-depth study of the background, variable health status and/or interactions of the patient in the hospital setting (Henderson, 1991). In keeping with appropriate case study protocol, multiple sources of evidence were used to create a chain of data from which to draw conclusions (Henderson, 1991).
HYPOTHESES
There is a functional relationship between TR and palliation, where participation in therapeutic recreation contributes to palliation in the advanced cancer patient.
SIGNIFICANCE OF THE STUDY
The significance of the study is that with increasing attention to issues of death and dying, role of health and medicine in improving the dying process, TR’s role may become increasingly important as a palliative treatment. Clinical observation and empirical research point to the importance of social contact and social support in the life of the dying patient (Breitbart & Holland, 1993). Indeed, TR can address many of the dying patient’s psycho-social, emotional, and physical needs and improve the quality of life, as it helps the dying patient maintain a positive attitude and sense of self (Willlets & Sperling 1983). TR can reduce fear through the supports engendered by psycho-social interaction, sense of accomplishment, physical activity, and reassuring continuity. TR increases a patient’s ability to gain a measure of control in the dying process. This study will increase the body of knowledge by demonstrating the positive benefits of TR with this population.
DEFINITIONS of TERMS:
PALLIATION
Palliation is a form of supportive care that is used by health care professionals when the course of cancer can no longer be significantly altered by medical interventions(Murphy, Morris, & Lange 1997). Treatment measures are administered to help the patient maintain the best possible level of physical, emotional, mental, spiritual and social life, regardless of how far along the disease has progressed(Murphy, Morris, & Lange, 1997). Palliative care is aimed at controlling symptoms and improving the quality of life in an effort to relieve symptoms, ease distress, and provide comfort(Murphy, Morris, & Lange, 1997).
TERMINAL ILLNESS
Terminal illness, such as advanced cancer, is defined as an illness that cannot be cured by present day medical technology and that generally leads to death within a specified period of time (Turk & Feldman 1992)
THERAPEUTIC RECREATION
For the purpose of this study, the definition of therapeutic recreation as written by the American Therapeutic Recreation Association will be used.
Therapeutic recreation is:
“The provision of treatment services and the provision of recreation services to persons with illnesses or disabling conditions. The primary purpose of treatment services which is often referred to as recreation therapy, is to restore, remediate, or rehabilitate, in order to improve functioning and independence as well as to reduce or eliminate the effects of illness or disability. The primary purpose of recreation services is to provide recreation resources and opportunities in order to improve health and well being. Therapeutic recreation is provided by professionals who are trained and certified, registered and/or licensed to provide therapeutic recreation” (ATRA, 1997).
CHAPTER II
REVIEW OF LITERATURE
The relationship between therapeutic recreation and palliation in the treatment of the terminally ill cancer patient is the focus of this study. There is very little in the therapeutic recreation literature on the use of therapeutic recreation in settings that serve the terminally ill. Connolly (1993) points out that although society has the tendency to abandon individuals with life threatening illnesses, TR professionals, traditionally concerned with the quality and potential of human life; need to face the realities of new illnesses and conditions that threaten life despite technological advances, and not lessen the quality of that life. Despite all the advances in medical treatment, some cancers cannot be cured (Cimino 1997). For these patients, TR may be particularly beneficial in the area of palliation. This review of literature will discuss palliation, the psycho-social impact of dying, the role of TR, and the quality of life.
PALLIATION
In 1995 the American Board of Internal Medicine, Clinical Competence Program distributed the following description of palliative care: at the “Conference on Care Near the End of Life”
“Palliative care is the active total care of patients whose disease is not responsive to curative treatment. Control of pain, of other symptoms, and of psychological, social, and spiritual problems is paramount. The goal of palliative care is achievement of the best possible quality of life for patients and their families. Many aspects of palliative care are also applicable earlier in the course of the illness, in conjunction with anti-cancer treatment.”(Cimino, 1997)
The World Health Organization (WHO) noted in 1993 that in certain member states there still appeared to be uncertainty about palliation, and therefore, stated that
“Palliative care affirms life and regards dying as a normal process. It neither hastens nor postpones death; it provides relief from pain and other distressing symptoms; it integrates the psychological and spiritual aspects of patient care; it offers a support system to help patients live as actively as possible until death; and offers a support system to help the family cope during the patient’s illness and in their own bereavement” (Cimino, 1997).
This study’s focus, palliation, is alluded to in the ATRA definition with the therapeutic recreation goal: “to improve functioning and independence, as well as reduce or eliminate the effects of illness or disability” (ATRA, 1997) This goal can have a palliative outcome.
THE PSYCHO-SOCIAL IMPACT OF DYING
Kubler-Ross(1969), the foremost authority on death and dying, was one of the first professionals to address this taboo subject. She interviewed many dying patients and discovered five stages of death and dying. These were (1) denial and self isolation; (2) anger; (3) bargaining; (4) depression and (5) acceptance (Kubler-Ross, 1969). She also recognized a universal fear of death, hope, a search for meaning, and a resurgence of spirituality (Kubler-Ross 1969).
The terminally ill all grieve their own death and the loss of family, friends, love and life. Kavanaugh (1972) categorized the grieving process into seven emotional states: (1) shock; (2) disorganization; (3) volatile emotions (4) guilt; (5) loss and loneliness; (6) relief; and (7) resentment.
According to Rando (1984), it is common for the dying patient to experience rejection, isolation, anger, anxiety, and feelings of abandonment. The patient usually begins to employ ego-coping mechanisms including repression, denial, rationalization, projection, intellectualization, and obsessive-compulsive behaviors.
Taylor (1992) examined the search for meaning among persons living with cancer. This was a cross-sectional study of 74 recurrent cancer patients. The following standardized scales were used in the study: (1) the Purpose of Life Scale; (2) Symptom Distress Scale; (3) Enforced Social Dependency Scale; (4) and the Psycho-social Adjustment to Illness Scale. Ten of these subjects also received semi-structured interviews which provided in depth qualitative data suggesting that persons experiencing negative or unexpected life events, such as cancer, reported a search for the meaning of life. The findings indicated that adjustment to illness was positively correlated with a sense of meaning.
In another study, conducted in 1993, of 195 women, it was found that causal thinking and perceptions of control were associated with the psycho-social adjustment of women with breast cancer (Lowery, Jacobsen, Ducette, 1993). The findings indicated that clinicians who work with cancer patients should be alert to possible adjustment problems because perceived loss of control is a predictor of psychological distress(Lowery, Jacobsen, Ducette, 1993).
Cohen coined the term “psycho-social morbidity” to describe the negative influences triggered by cancer. A malignancy is a massive assault on the physical and psychological integrity of the person (Aaronson & Beckman, 1987). It includes the distress the patient experiences at all stages of the disease beginning with a diagnosis of malignancy, through death. For the patient, the combination of surgery, radiation, chemotherapy, or the choice of receiving no treatment, each present special terrors. Functional impairment or disfigurement from cancer, treatment or both is a threat to one’s bodily integrity. Neoplasm (excessive tissue or tumor growth) and physical sequelae (the disease process)pose a threat to one’s previously held self-concept and frequently necessitate changes in self-image (Aaronson & Beckman, 1987). Issues of loss and the development of clinical depression are inevitable.
Aaronsen & Beckman (1988) refer to the buffering effect of social supports. Their research findings maintain that the health and mental health benefits of social supports are evident during periods of high stress associated with cancer. Social support, a potential outcome of therapeutic recreation interventions, can be a reserve or resource, which enables the individual patient to cope more effectively with the disease process (Aaronsen & Beckman, 1988).
ROLE OF THERAPEUTIC RECREATION
Given the above psycho-social issues, the following are four problem areas of dying patients can be addressed through therapeutic recreation: 1)Uncertainty: goals are written to increase the patient’s psychological comfort and to keep some dimension of hope alive until the end of life (Rando, 1984); (2)Negative feelings: goals are written to divert attention away from the stress and fears associated with the disease in an effort to reduce anxiety and depression and to address feelings of sorrow shame and loneliness (Aaronsen & Beckman, 1987); (3)Control: goals are written to facilitate a restored sense of control and accomplishment (Rando, 1984); and (4)threats to self esteem: goals are written to foster participation in groups enhancing peer supports, and the opportunity to pursue new and old leisure interests (Aaronsen & Beckman, 1987).
Willetts and Sperling (1983), list the goals and objectives of therapeutic recreation in serving the advanced cancer patient this way: (1)to educate or re-educate patients in the constructive use of their leisure time, during hospitalization and/or after discharge; (2)to eliminate boredom and as a result, to help alleviate stress and anxiety; (3)to provide a variety of unique recreation and cultural opportunities to patients; (4)to help patients regain or reinforce their self esteem through recreation experiences; (5)to provide emotional and psycho-social support to patients and their families; (6)to adapt leisure activities for patients, based on their physical and emotional needs; and (7)to continue, as much as possible, the patient’s normal leisure activities during hospitalization.
Therapeutic recreation is a useful adjunctive or complementary therapy for the advanced cancer patient and can produce outcomes which improve a patient’s perceived quality of life. Quality of life is the balance between euphoric and dysphoric feeling states (Aaronsen, Beckman 1987). Physical illness and impairments from advanced cancer lead to a perceived reduction in the quality of life, and a notable increase in anxiety, uncertainty about the future, and other dysphoric feeling states (Aaronsen, Beckman, 1987). Adaptation to life with cancer may be relative to the reduction of dysphoric emotions and the creation of a life situation with adequate resources for personal gratification(Aaronsen & Beckman, 1987).
An oncology therapeutic recreation program was established in a 20 bed clinical research unit at Duke University Medical Center that provided leisure education, companionship, games, crafts, music, trips and group activities (Bost & Brown, 1982). Here, with recently diagnosed patients, therapeutic recreation was found to be a process which is rehabilitative in nature as it helps to relieve stress, anxiety, and boredom (Bost & Brown, 1982). It provides outlets for the expression of emotions, opportunities for socialization, and creativity (Bost & Brown, 1982). The patients are considered survivors and are encouraged to live their lives as fully as possible (Bost, Brown 1982).
Leisure awareness, an important concept in therapeutic recreation, is imperative at the end of the life cycle. Lahey (1993) writes that the threat of death poses the greatest possible challenge to one’s identity. She states that those leisure pursuits which have contributed to a person’s self-identification will be particularly meaningful now and can provide a “saving balance” in the midst of illness (Lahey, 1993). Leisure education plays an important role in working with advanced cancer patients. It assists people in gaining and maintaining leisure activities and experiences that contribute to their quality of life, to the very end of life (Stensrud, 1993).
Originally designed to describe the function of leisure in relation to work, the compensatory theory of leisure suggests that an individual will seek the opposite type of activity whenever given the opportunity to avoid their regular routine (Neulinger, 1981). In a hospital setting, getting to appointments on time and enduring various treatment regimens such as palliative radiation, X-rays, bathing, and eating can be like work in that everything is task oriented. It is, therefore, important to determine the patient’s perception of their daily routine and various appointments in order to make appropriate recreation choices.
The familiarity theory of leisure assumes that most people work out comfortable routines for social survival producing a sense of security (Neulinger, 1981). Advanced cancer is a serious threat to this and research suggests that the patient no longer has the social network to experience social recognition, which may lead to feelings of loneliness, isolation, and boredom (Aaronson & Beckman, 1987). The dying need continued and rewarding interaction with others as uncertainty brings increased anxiety and fear. Therapeutic recreation activities can help patients develop comfortable routines in the hospital and increase opportunities for socialization and life affirming interaction (Willets & Sperling, 1983).
The personal community theory further accentuates the social properties of leisure where an individual’s psychological drives and desire for social contacts with others become satisfied indirectly through activities shared with friends, family, and co-workers (Neulinger, 1981). The importance of one’s social support system is crucial to palliation, and therapeutic recreation can increase social support (Bost & Brown, 1982). Therapeutic recreation is a modality that can offer patients the opportunity to engage in leisure based activities individually, in a group, or in a therapeutic community. Research, done in a medical model setting, also suggests a positive relationship between social support and the rehabilitation of a cancer patient (Aaronsen & Beckman, 1987).
Families or caregivers may receive TR services in the form of respite, support, and actual involvement in TR activities with their loved ones within TR programs. Current oncology therapeutic recreation programs approach treatment in an eclectic manner to best address the needs of the patients they serve. One pilot program studied the value of a pet therapy program for terminal cancer patients in a nursing home(Muschel, 1984)and found that the experience of being with the animals had an effect of creating a sense of relaxation and reducing tension and a reduction in blood pressure (Muschel, 1984). Using a questionnaire, it was found that pet therapy increased the comfort and adaptation of the dying patient(Muschel, 1984).
Research on the effect of other therapeutic recreation activities such as the above is needed. Research with adult cancer patients has shown that patients can be trained in specific relaxation and stress reduction techniques to control their own anxiety, and to reduce pain and stress during invasive medical procedures (Breitbart & Holland, 1993).
The recreation therapist plays many roles in an oncology setting; assessing the patient’s functioning, establishing goals and objectives, designing an appropriate treatment plan, evaluating each patient’s progress and enhancing the patient’s personal capacity to cope with the disease process (Willetts & Sperling, 1983). Stensrud (1993) writes:
“The therapeutic recreation professional has a responsibility to address death in order to help people live fully until they die. It is our responsibility as professional recreation therapists to address the sensitive subject of death awareness because we often have the best opportunities to do so. We are frequently called upon to be the confident of our clients. We connect with their expressive domains and encourage cathartic release of emotions through re-creative activities. We are present at some of the most powerful occasions, when, for example, the magic of the leisure experience can open a person to poignant insights.” (Stensrud, 1993, p.36)
This can occur in groups or at bedside through activities that address life and death issues through symbolism, interaction, and reflection. Indeed, experiences and insights are difficult to measure but, as therapists, we are called upon to facilitate the process, and, hope to be a catalyst in helping patients achieve goals and receive the benefits of therapeutic recreation.
THERAPEUTIC RECREATION, PALLIATION AND THE QUALITY OF LIFE
Therapeutic recreation can improve functioning, increase independence, address psycho-social issues and reduce the perceived threat of terminal illness through a choice of leisure activities, that cause a palliative outcome. Palliative care is a treatment modality provided for patients who are not curable, in hopes that treatment interventions will relieve or alleviate symptoms such as pain and anxiety, without altering the course of the disease (Stoll, 1986).
There is very little research in the literature measuring a the causal relationship between therapeutic recreation and palliation. Research measuring a patient’s adjustment to illness and quality of life, however, is well documented (Aaronson & Beckman 1987). To study the use of therapeutic recreation in a setting where the quality of life is limited by the ravaging effects of cancer can be done through case study, quality of life surveys, patient adjustment to illness surveys, and patient satisfaction surveys used by researchers studying the quality of life of cancer patients (McDowell & Newell, 1996).
The case study (or case history) is found to be useful for collecting subjective data regarding a single case and the surveys are useful for the study of large groups of patients (McDowell & Newell, 1996). Given that there are so many uncontrolled variables in the hospital setting, a case study is considered the best approach to examine how TR goals and interventions serve the advanced cancer patient. TR goals and interventions appear to facilitate palliation when used with advanced cancer patients in that they help to maintain quality of life (Bost & Brown, 1982). Although there is little scientific evidence as to the effects of such treatment, the benefits of this approach centers on improving the quality of life through enhanced psychological support (Lerner, 1994).
The World Health Organization noted in 1993 that palliative care affirms life and regards dying as a normal process (Cimino, 1997). Palliation provides relief from pain and other distressing symptoms, offers a psycho-social support system to help patients live as actively as possible until death, integrates the spiritual and psychological aspects of patient care, and provides support to the family during the patient’s illness and following their death (Cimino, 1997). Palliation includes the reduction of pain through medication such as morphine, bereavement services to the patient and family, unlimited visitation policy, availability of pastoral care, and holistic and more non-traditional forms of medicine, as well as therapeutic recreation services.
CHAPTER III
METHODOLOGY
RESEARCH DESIGN
The design of this study is a case study which is an extensive description of a single individual in order to generate a hypothesis which may be applicable to many other patients following the completion of further research (Davison & Neale, 1996). Korchin (1976) lists the obvious limitations of the case study as: (1) uncontrolled, (2) often unsystematic, (3) generalized and uncertain, and (4) the observations and conclusions can all too often reflect the subjective judgment and bias of the observer. Through the case study, however, the researcher can observe the full complexity of human responses and behavior (Steuer, 1994). This case study attempts to comprehensively describe the relationship between therapeutic recreation and palliation for one advanced cancer patient.
MEASURES & INSTRUMENTS
This case study used several of instruments to collect data for the case study including notes which were processed daily, the Calvary Hospital TR assessment and the Functional Assessment of Characteristics for Therapeutic Recreation. The Calvary Hospital assessment was the initial assessment tool and it was used to establish a socialization goal and objective for the patient. This assessment was conducted one day after interviewing the patient following her admission and was entered into the chart. The Calvary Hospital TR assessment provided general information including her age, family information, significant physical information including her diagnosis, physical needs at time of assessment, her mental status regarding reality orientation, and present recreation interests.
The Functional Assessment of Characteristics for Therapeutic Recreation(FACTR) was used once a week over a three week period in an effort to gain a broader perspective of the patient’s functional status and to determine if any changes could be noted. This assessment measured the physical, cognitive and social/emotional domains of the patient using three respective eleven point scales. Only one of the questions was not applicable to the study and that was Math Concepts. The patient may have been able to engage in mathematical exercises but the opportunity to do so during this study did not present itself.
Three weeks of daily TR process notes were collected by the researcher during the study. These were based on behavioral observations of the patient during TR and are presented later in this paper.
DESCRIPTION OF THE SETTING
From its inception in 1899, the mission of Calvary Hospital has been to provide palliative care to adult patients in the advanced stages of cancer, addressing the symptoms of the disease, not its cure. Calvary Hospital is a voluntary, not-for-profit 200 bed fully accredited specialty hospital that is dedicated to providing patients with advanced stage cancer a comprehensive palliative care program that strives to meet the emerging physical, psycho-social, and spiritual needs of both patients and families through the provision of inpatient, outpatient and home care services.
Each patient has his or her own private room which is equipped with a reclining wheel chair, television, video cassette player, bulletin board, bedside table, closet, indirect lighting fixtures, a rolling beside tray table, visitor’s chair, a large window sill, and, a modern electronic hospital bed. The rooms have oxygen and suction ports built into the wall above the bed. The walls are decorated with paintings and photographs providing an aesthetically pleasing environment.
Therapeutic recreation is provided at beside beginning with a bedside visit upon or shortly after admission. Therapeutic recreation programs are held in various day rooms and recreation areas throughout the building. The main recreation area and patient activity centers are located on the first floor. Patient rooms are located on the third, fourth, fifth, and sixth floors making elevator trips a daily event for patients who attend recreation off their unit.
Supplies for all activities are kept in the main recreation area, and in cabinets in the day rooms. The day rooms have one television, a stereo, and, are stocked with games and general craft supplies. A sampling of various activities and projects are displayed to motivate patients and generate interest in the therapeutic recreation program.
Patients receive therapeutic recreation services daily. Some attend groups, others participate only at beside. In 1996 Calvary Hospital had a total of 2,485 admissions and 2,218 expirations. The remaining 237 patients were discharged home or to a nursing home with 96 of those being readmitted. The average length of stay is 26.5 days, from date of admission to death or discharge. The median length of stay is 17.0 days. About 890 patients,(35.7%), had stays of less than nine days.
This patient lived beyond the average length of stay at Calvary Hospital given that she was admitted on 8/11/97 and expired on 12/25/97. In total, she lived at Calvary Hospital about four and one half months. This fact demonstrates how difficult it can be to predict life expectancy at the end stage of the illness.
SUBJECT SELECTION
The patient was chosen out of a pool of 18 other potential subjects who attended group TR programs at Calvary Hospital up to four or five times per week. Four patients were told about the study and were asked if they would like to be involved in the researcher’s research project. The patient who was chosen readily agreed to participate and signed a release. All of the potential subjects were told in simplified terms that the purpose of the study was to understand the experiences of an advanced cancer patient in therapeutic recreation and TR’s relationship to palliative outcomes.
The specific palliative outcomes to be observed included active/passive social interactions, accomplishment of various sequential task oriented activities during TR, frequency and level of participation and observed behaviors such as attending to structured activities, interacting with peers, talking, laughing, and engaging in self directed activity during TR. The data reflect the sequence, nature and pattern of the patient’s engagement in various recreational activities during her first three weeks of hospitalization.
The timetable for the study was set for three weeks from the date of admission to the hospital. Given that the length of stay is usually less than a month, three weeks seemed like a reasonable amount of time to study an individual patient.
The first week was used to establish a baseline which was followed by two weeks of continued TR interventions. The patient freely chose which TR programs to attend. Given that the patient continued to live beyond the study period, a follow up interview regarding TR was also conducted.
To implement the study the researcher observed the patient during TR on a daily basis in a way that was as unobtrusive as possible. The researcher observed from the back of the room and discreetly took notes which were later compiled and processed. Every effort was made to maintain a “normal” patient/therapist relationship and the patient was observed participating in TR through a variety of group and individual programs. No special treatments or extraordinary interventions were provided and the routine of providing TR was no different for this patient than that for any other.
DESCRIPTION OF THE PATIENT
The patient was a 67 year old female who was admitted to Calvary Hospital on 8/11/97. She transferred from another hospital due to the progression and incurable nature of her cancer. She was first diagnosed with cancer of the larynx in May 1996. At the same time patient was found to have cancer of the right breast. She had a lumpectomy but chose to receive no radiation for it.
The patient did receive radiation and chemotherapy for the cancer of the larynx, at which time, a fistula was fixed internally. She had a complication from the chemotherapy, with cardiac arrest and had subsequently refused surgery. She agreed to have a PEG feeding tube put in place; later she experienced greater difficulty breathing and required a tracheotomy. The patient developed some form of heart disease and was also seen by a psychiatrist for suicidal ideation. At time of admission she appeared more agitated then depressed. She reported some persistent pain despite use of Percocet.
The patient was married with two adult daughters. Her general appearance was that of a well developed, normally nourished woman. She had a history of heavy alcohol use and smoked two packs of cigarettes daily. She was selected for the case study shortly after her admission to the hospital. She was a typical end stage cancer patient who had arrived from another hospital to receive palliative treatment. Since her previous hospital did not provide TR, she needed to be educated about the TR program, provided with a calendar, told about her choices and options regarding TR, including the benefits and supports that can be gained in TR groups.
The patient was informed of the research project this researcher was doing. She was told that this researcher was conducting a study to determine the benefits of Therapeutic Recreation for advanced cancer patients and that the problem was to determine if TR contributed to palliation. She was told that this study would keep her full name confidential and that she could withdraw from the study at any time. She agreed to participate in the study and informed the researcher that she was a teacher and thought that maybe the research could help in some way.
The patient was assessed by using the Calvary Hospital TR assessment as well as the Functional Assessment of Characteristics for Therapeutic Recreation(FACTR).(See Appendix II.) Note regarding her process notes, reported below, were recorded daily following her participation in both individual and group interventions. Days when the patient did not participate are noted as such.
CHAPTER IV
RESULTS
The purpose of this study was to investigate the relationship between TR and palliation in the treatment of the patient with advanced cancer in a clinical setting. The problem of this study was to find a causal attribution between TR and palliation; in that TR contributes to palliation by reducing or relieving symptoms of the disease, increasing appropriate functioning, and increasing a patient’s ability to cope with dying. Included in the study was an attempt to find a causal attribution between TR and palliation through the patient’s involvement in therapeutic recreation. The analysis of the data is presented in this chapter according to the following topics: (1) The Calvary Hospital Assessment, (2) The FACTR assessment, (3) daily notes regarding the patient’s activity level during these therapeutic recreation, (4) a Table which lists the patient’s level and frequency of participation in TR the three week study and (5) a post test interview with the patient.
The research process began with a reality orientation pre-assessment visit from the researcher who was also the covering recreation therapist. Information about TR programs was provided to the patient and the patient herself subsequently provided valuable information that would later be used in conducting both the Cavalry Hospital TR Assessment (see Appendix I) and the three Functional Assessments of Characteristics for Therapeutic Recreation (see Appendix II).
The Calvary Hospital Assessment revealed a patient who was alert, responsive, verbal and fully oriented. She spoke in whispers but, could make her needs known. She appeared interested in the TR and expressed a hope to “go out soon”. A goal for socialization was entered into the chart based on this assessment.
The Functional Assessment of Characteristics for Therapeutic Recreation(FACTR) was used three times, once each week, to further assess the patient as well as to monitor her progress. This assessment measures the physical, cognitive, and social/emotional domains and can be used to determine a patient’s needs and/or changes in functional ability. The findings of most interest for TR were found under the social emotional categories. In the dyad situation(3.2) the patient appeared to have made progress in that she was initiating situations and conversations in just over two weeks. She often stated that being involved helped her to feel comfortable and gave her a sense of purpose. By initiating interactions during TR with peers, the patient was able to develop supportive friendships that appeared to help her cope with her disease.
The small group interaction category(3.2) also showed a positive change from being on the sidelines to initiating independently. When the FACTR was administered the first time the patient behaved more as an observer and responded only minimally. Her conversations were limited in duration. When the assessment was conducted 16 days later the patient was attending TR daily.
DAILY PROCESS NOTES
WEEK #1:(8/11/97-8/17/97)
8/11: Admitted to Calvary Hospital
Today the patient was admitted. She received visits from all the disciplines including TR. Upon approach the patient presented as being dependent on oxygen and short of breath. This was an introductory visit to briefly orient the patient to TR services.
The therapist/researcher briefly described available TR programs and how patient could access the service. She was provided with the daily TR schedule and told about various self directed options available including the video player, movie library, games and access to the outdoor terrace. She seemed polite and mentioned she needed to rest. She agreed to a follow up visit from TR staff.
8/12: Initial Assessment Visit, 1:1, 15 min.
The patient was resting in bed, she had oxygen running, and presented as being alert, anxious, and irritated. She rapidly scanned the therapist with actively moving eyes and she expressed a degree of assertiveness by saying she was not interested in recreation activities, at least not yet. She asked what day of the week it was. She appeared to question it being a Tuesday afternoon, but nodded her head in agreement. She covered her tracheotomy as she spoke, in barely audible whispers of not being able to eat, walk, or get out of bed.
She accepted another therapeutic recreation activity schedule, and seemed to be listening attentively as various programs were described. She clutched her oxygen line and said that because of it she was unable to do anything, and would most likely remain in her room. The therapist took this as an opportunity to explain that if she does begin to feel better she may decide to join a TR group and that oxygen tanks would be provided. Or, for the time being she could choose to watch a TR movie in the room, or do a number of various TR activities in the room.
She appeared to understand that being involved with recreation was an option available to her when the need arose. She remarked that she needed to rest but, agreed to future visits from the TR staff.
8/13: Patient/Family Education, 1:1, Pt. & Spouse, 10 min.
Today the patient was out of bed and sitting in a lumex chair.
This is a special reclining wheelchair that is provided by the hospital. (This type of wheelchair is not designed so that the patient can propel it on her own. Only a few patients ever use a traditional chair.)
She had the oxygen going and was holding a yellow pad with a pencil in her lap. During the conversation she used the pad to express herself from time to time. She wrote quickly and with determination. She passed the pad back and forth to the therapist as the visit proceeded. She seemed comfortable communicating with a mix of oral verbalizations and written scribbles about her choices in TR. She said that she would possibly attend Arts and Crafts later during the day but, would have to check to see if her husband would be coming in to visit.
The purpose of this morning visit was to motivate and provide the patient with information regarding the day’s program. Arts and crafts is held every Wednesday afternoon. She asked how much it cost and was informed that all recreation programs are free. The therapist suggested that there were benefits from attending recreation, and that seeing other patients provides an element of support as well as a chance to socialize.
She pointed to the oxygen and asked “What about this?” The therapist explained that portable oxygen was available and could be brought to the program. “How do I get there, I can’t walk?” she asked. The reclining chair has wheels as the therapist demonstrated by rolling it back and forth. She was told that a volunteer or TR staff member would happily bring her to the program. She did not agree to go to the program at this time but, later in the day, did accept an “invitation” to attend. She was assured that there would be plenty of oxygen in the tank. She listened as the therapist said that if at anytime she wanted to return to her room, she could.
8/14: Patient assessment, goal, objective, plan of care: As per hospital policy a departmental TR assessment was entered into the medical record. See Appendix (I)
This initial assessment is used to determine measurable TR goals and objectives and is subject to revision as needed. Goals and objectives are systematically evaluated by therapist every ten days. Goals and objectives are written following an assessment visit as presented below.
Today, before writing goals and objectives for patient regarding TR participation, the patient accepted a socialization visit. The patient was breathing freely without being “hooked-up” to oxygen and had been given permission to smoke in the day room. A doctor’s order is needed for a patient to smoke. Once an order is written the patient is allowed in designated areas such as the dayroom or outdoor terrace. Cigarette smoking is not allowed in patient rooms and cigarettes are kept at the nursing station.(The conflict between smoking and going to recreation had ramifications that will be discussed below.) The smoking privilege pleased the patient and she later skipped recreation so that she could subsequently smoke in the day room instead of attending ceramics which, like all indoor TR programs, is an activity where smoking is prohibited.
The patient had not had a cigarette in weeks and it seems her previous lack of freedom to smoke limited her desire to attend TR. This was reflected in TR chart notes but, was not apparent during the initial goal setting phase of her TR assessment. Following a discussion with the patient, which included a review of the various opportunities she had regarding TR, the goals and objectives were written on the TR assessment and entered into the medical record as follows: ....................
GOAL STATEMENT: To increase socialization.
OBJECTIVE #1. Pt. will accept daily visits 3-5x weekly. OBJECTIVE #2. Pt. will attend TR group(s) of her choice 2-3x weekly.
PLAN: Provide TR services and supports to patient and family. Collaborate with interdisciplinary team and discuss progress at weekly team meetings. Bring portable oxygen along to program as needed.
8/15: Horticulture Program on terrace: 60 minutes.
Today patient attended the TR horticulture program on the terrace from a distance. She asked to sit in a shady area away from the group in an area where other patients usually smoke. She focused on smoking but was scanning the terrace and appeared to be taking it all in. Her husband sat near her, carried a paper, and seemed comfortable as the afternoon progressed.
The patient also met other patients and seemed to be inquisitive as to who they were. Most were fellow smokers and smoking behavior on the terrace is noted here as a chance for the patient to interact with peers as well as to observe TR’s horticulture group.
8/16: No formal TR interventions provided.
One of the patient’s daughters was visiting. Together in the dayroom with her husband present, the patient was sitting in her wheel chair, smoking.
8/17: Supportive Visit, 1:1, 10 min., Motivational Rounds, 1:1, 5 min.
Patient accepted a visit from TR staff and agreed to attend TR later in the day.
8/17: Group Games: 90 minutes
Patient accepted invitation to attend a Pokeno game on the terrace. She was successful and won some prizes as she engaged in this out-door activity that is played much like bingo. Following the game the patient remained on terrace to smoke and she was interacting with other patients and their visiting family members.
WEEK #2 (8/18/97- 8/24/97)
8/18: Supportive Visit, 1:1, 10 min., Motivational Rounds 1:1, 5 min. Group, Creative Arts: Puzzle Making, 60 min.
Patient made an effort to make a cut-out puzzle kit where a blank pre-cut puzzle is painted with a design of the participants’ choosing. The patient had some difficulty manipulating the brush and acrylic paint, reflective perhaps, of a decline in fine motor skills as a result of the disease process and/or medication. Claiming she was no artist, she made a simple design with minimal assistance but required a recreation therapist to help her complete the project at bedside the next day.
She worked alongside other patients and interacted with them in a socially appropriate fashion. She asked a question about one patient expressing concern that the patient was absent from the group. TR was the primary time that the patient was in a group with other patients. When other patients were not available for TR, this patient often asked about those who were not in attendance.
She appeared anxious as evidenced by her standing up and holding on to the table, yet she made eye contact with concerned staff and assured them she was “OK” on her feet. Standing attracted the attention of her peers as most of the patients in attendance were unable to stand up on their own. Her act of standing seemed to reflect her desire to achieve a level of independence.
(It should be noted that the patient had earlier declined a physical therapy consult to assess her ability to ambulate. Recreation therapy appears to be the way she desired to improve her physical functioning and she told the recreation therapist as much on several occasions. She eventually was allowed to walk to programs as long as a staff member or volunteer brought her chair in tow. Subsequently, on 8/30/97, her doctor wrote an order whereby she was allowed to ambulate on her to the dayroom, as long as she agreed to hold on to the hand rail.)
She did not have any snacks or refreshments during the session. Throughout her stay, the patient never ate snacks, and the psycho-social impact of this is noted later in the study.
Although she did not finish her puzzle project on this day, she stayed on to smoke and socialize until she became the last patient to go back to her room.
8/19: Supportive Visit 1:1, 15 min., Creative Arts Visit 1:1, 15 min. Bingo 90 min.
Today the patient appeared distressed and accepted a supportive visit where she expressed frustration at being sick. The therapist encouraged her to come out for Bingo and she agreed to give it a try. She attended a Bingo game on the terrace later in the day. During Bingo she was alert and participated having her husband call out if she had a winning card. She actually won a blanket and seemed to be in good spirits. Following Bingo she joined what was to become a small socially active smoking group. The patient was observed providing a cigarette for a fellow patient who had none. The quiet conversations among this sub-group appeared serious but friendly and supportive.
8/20: Motivational Rounds 1:1, 5 min. Group, Arts & Crafts, 90 min.
Patient attended arts and crafts today, did no “work”, but rather observed and interacted. She left the group to smoke after 40 minutes. The total time was spent chatting, smoking, and watching other patients. Her interest in other patients and their respective situations seemed to compel her to interact.
8/21: Group: Music Appreciation, 60 min.
Music appreciation is held in the morning and this patient smoked before the program, only putting out her cigarette when a patient with oxygen was brought into the session.
Later, she did not attend ceramics but was observed up on her unit, smoking in the day-room. Her husband was keeping her company near by.
8/22: TR Group: Horticultural Therapy-Dish Gardens, 90. min.
Patient had no visitors and accepted an invitation to attend Horticulture. The project was to make a dish garden where the patient selects a ceramic dish, assorted house plants, and the items needed to make a mini-garden.
The patient said that she had no luck with plants. She said everything she ever grew died. The therapist explained that this was a project that could be used as a gift. The concept of the living legacy of plants was also discussed. This is the idea that the plants can actually be a living legacy of the person who planted them.
The patient made two planters independently. It seemed that her fine motor skills using small hand garden tools were adequate for this activity. Although this was a sequential task oriented process, it did not require exacting techniques of Arts & Crafts and she did quite well planning and planting her dish gardens. She carefully added drainage material, soil, water and small plants into the container with little difficulty. She wore gloves as she mixed the soil and her eyes continually darted about the room. She stood to do up her project and she balanced herself against the table. Staff came over to her to make sure she was stable and she seemed annoyed by their presence.
The patient said she was going to give one of her dish gardens to her daughter in Philadelphia who “loves plants”. She planned to keep one in her room to try her luck once again with growing plants.
8/23: Social Group: 90 min.
Patient had her daughter, son-in-law, and grand children with her as she attended a large social group on the terrace. This was a generally informal program where patients visited with peers or loved ones while sharing food and refreshments.
The patient saw a young patient across the way and asked the therapist if she could bring her grandchildren over to her to introduce them. TR informed her that he would check. A short time later the patient was introducing her adult children and grand children to the young patient. She introduced the young patient to her family as a good friend. Indeed, the young patient smiled and seemed quite equally friendly toward the patient.
8/24: Supportive Visit: 10 min., Special Event: Magic Show on terrace, 90 min.
The patient attend a magic show on the terrace. She socialized and interacted with both her family and the other patients. She stayed following the show and smoked three cigarettes.
WEEK #3:(8/25/97-8/30/97)
8/25: Supportive Visit, 1:1, 15 min., Relaxation Group 60 min.
Today the patient attended the relaxation and movement group. This program incorporates guided imagery with relaxation and movement of the upper body. The patient joined the group in a circle and held on to the parachute as it gently floated as instructed. She participated for about 60 minutes before returning up to her unit for a smoke. For one hour the patient had not had a cigarette but it seemed that smoking was an important aspect to her quality of life. Smoking perhaps gave her an added element of control, something to do on her own following TR.
8/26: Life Review, 1:1, 15 min.
Today the patient accepted a one to one visit which is used to help patients realize a life affirming continuum. The patient shared some aspects of her past. She reflected on her years as a teacher, mother, and one who always felt she could have done more. She claimed to have once considered going back to school for social work and lamented it was now too late. Her leisure apparently was centered on her family. Her history of smoking and drinking did not come up in the conversation. During this visit the patient used a pad and pencil to communicate. She was having trouble with incessant coughing and oral verbalization was minimal. The therapist encouraged her to go to bingo once again and assured her somebody would assist her to call out Bingo if she won a game.
8/27: Group, socialization on terrace.
Today patient chose not to attend the Arts & Crafts program, but did join peers on the peripheral part of the terrace where smoking and independent socializing was occurring. The TR program was hat decorating and the patient did not even attempt to participate in the required multi-step task oriented process.
8/28: Motivational round, 10 min., Group: Music Appreciation 60 min.
Today patient attended Music appreciation and she stated that she really liked the old big bands and songs the most. She listened to the music and reflected on some of her memories as the program proceeded. She said music will never be like that again. She held off smoking but seemed thrilled when the session ended so that she could smoke again as evidenced by her immediate smoking behavior. She had asked during the session if she could smoke and was told “not until the session was over”.
8/29: Group: socialization on terrace, 90 min.
Today patient chose not to attend the horticulture group but did come down for smoking and socializing with peers on the terrace. She walked with assistance over to the group, observed the program for a few minutes, and declined an invitation to join it before retreating back to her chair and fellow smokers. She sat in her chair puffing and whispering intermittently for almost 90 minutes and she again was one of the last patients to return to her room.
8/30: Labor Day Party, 90 min.
Today the patient’s doctor signed an order that gave the patient a greater degree of control. He granted the patient the right to ambulate on her unit. This meant that the patient could now engage in increased self directed leisure as she could go on her own to the day room. The patient herself had sought this and was already ambulating to some degree.
Later in the day the patient attended a Labor Day Party. She ambulated on and off throughout the program, mingling with peers as a friend.
During this party it was difficult to observe all of her interactions, in general terms however, she integrated well as she greeted her hospital friends, and introduced them to her family and her grandchildren.
The patient watched as her grand children ate hot dogs and seemed sad, nervous and anxious at the same time. She was on her feet pacing back and forth, lighting cigarettes, smoking, grimacing, and reaching out to the children with her hands. Later she complained that she could not eat but she was glad her guests could. (As noted earlier above, she has a feeding Peg tube and receives food via a nutrient pump.)
Following the party she presented one of the planters she had put together in TR to the daughter who loves plants. The patient seemed pleased and proud to be the person who made a dish garden. Her daughter promised to take good care of it and the patient said “I know she will”.
Table 1: TR interventions during the three week study period is presented below:
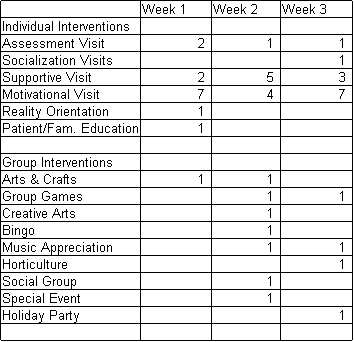
POST TEST TR INTERVIEW: Conducted 10/1/97
Since the average life expectancy at Calvary Hospital is less than 22 days, and the fact that the subject continued to live for many days beyond the study period a follow-up interview, reported below, was conducted on October 1, 1997. This interview took place in patient’s day room. The questions were written to elicit responses congruent with the focus of the study:
1. From your perspective, could you please describe therapeutic recreation?
“The recreation therapists are all very concerned. They have helped me meet people here I never would have known otherwise except that we met in therapeutic recreation.
2. You seem to have described TR by actually describing the TR staff?
“Yes, I have developed such a bond with them and I never would have been their friend before I got sick. Now I have friends also who are so different than me, you know other patients and it helps me get through with this cancer. I ‘ve met these friend at recreation.
3. So meeting people at recreation helps?
“I still sometimes wake-up and say it’s all a bad dream, but it doesn’t last long. I get sad and it’s kind of lonely.
But through recreation, and meeting other people, I make the best of it.”
4. What do you do when you go to recreation?
“I’ve made so many gifts for my children. My daughter, I made her ceramic cats. She loves cats. I made something I knew she would like. She lives in Florida, and she keeps it on the kitchen table. I also made some planters at ceramics and then in horticulture I filled them with plants. These I gave to my other daughter, in Philadelphia, she loves plants and this gives me a sense of responsibility. It helps me feel like I’m still able to do things”
5. So you like to make things in recreation that you can use for gifts?
“Yes and I give them all to my daughter, I give them all away. She loves plants so she can have them.”
6. Before this did you have any interest in houseplants?
“No, I had no previous interest in plants, until now, not until I came here“.
7. Have you developed any other new interests?
“In ceramics, I made my three grandsons a pumpkin and filled it with candy, then sent it to the boys. I look forward to starting something even though it takes me days to finish.”
8. What else have you done in recreation?
“In crafts I made a cigarette case. What I win in Bingo I give away. I give away everything. There is nothing in my room.”
9. How does therapeutic recreation help you deal with your illness?
“I’m not in much physical pain but, it helps with my emotional pain. If you have to be in a place like this, with cancer, there’s no other place like this in the world, it helps.”
10. Can you describe your relationships that you have developed with other patients you have met in recreation?
“I like to get involved in other people’s lives, to be a good listener. I like people. Therapeutic recreation gives me a chance to be involved. I’m a people person and I’m very interested in people. Here’s an example of how recreation allowed me to meet people and why everybody knows Barbara. I met [Cynthia], and she opened up to me. We were both making stained glass during crafts. She told me about her troubles, and about her child who was missing at the time. I told her about myself too. Now I look for her and she looks for me at recreation. I got involved with her life to the point that her boyfriend once came to visit me. He even took me for a smoke.” This was the last question and the patient returned to her room to rest.
This interview was conducted to get subjective data from the patient several weeks following the study period. The data reflects the patient’s continued participation in therapeutic recreation. She appeared to appreciate her relationships she had with TR staff and said that she had bonded with them. Then she described some of her peer relationships and the importance of being friends with people who she never would have met had she not become ill. She spoke of the importance of having the time to finish her projects in TR and the joy of sharing them with her family. Finally, she discussed how everybody knew who she her which reflected a positive sense of self in the face of impending loss.
CHAPTER V
CONCLUSION
Therapeutic recreation and therapeutic recreation activities appeared to contribute to palliation in treatment of this advanced cancer patient. TR interventions helped the patient increase her sense of accomplishment, reduced her depression, minimized her threats to self esteem, and put real fears in perspective. TR alleviated or reduced her distress and anxiety through outcome based TR interventions that increased psychological support, decreased social isolation, promoted socialization, rebuilt self esteem, increased independence, and maximized functioning making it a vital and integral treatment in a palliative care environment.
Following her admission to the hospital the patient accepted supportive visits from the TR team and was attending group activities within several days. She achieved her TR goal as evidenced by her acceptance of daily socialization visits 3-5 times weekly and her attendance at TR programs off the unit 2-3 times a week as well. During the first week, or baseline phase of the study, the patient attended three TR programs: arts & crafts, group games and creative arts. She accepted eight bedside visits of which four were motivational rounds, two were supportive visits, one was an assessment visit and one was a bedside reality orientation session.
During the next two weeks the patient attended TR groups on all but two of the days. She tried every program being offered during this time and engaged in some self directed socialization activity (sitting on the outdoor terrace during TR, not participating in the planned activity, talking and interacting with peers.)
Therapeutic recreation helped the patient maintain a relatively independent quality of life. During this three week study the patient made many independent choices about which programs she would attend. She developed supportive relationships with peers during TR. This illustrates the research of Aaronson & Beckman, (1987) who conducted studies regarding how the buffering effect of social interactions help a cancer patient cope more effectively with the disease process.
Psycho-social supports helped the patient deal with self isolation. The patient chose certain days not to attend any recreation program and in a sense, isolated herself from the group. This self isolatory behavior can be expected and is discussed in the literature by both Rando, (1984)and Kubler-Ross (1970). Most days, however, she accepted a supportive socialization visit from the recreation therapist and later that day chose to be present during recreation programs. The fact that she did not always engage in the structured activity reflects an element of personal decision making and illustrates her ability to maintain a continuum of self directed activity.
The threat of death posed a threat to the patient’s identity. Her acceptance of death and the dying process itself is reflected by the patient’s need to give away or leave behind numerous projects that she made during TR. By providing her loved ones with “gifts” she made in TR, the patient demonstrated her personal acceptance of her impending death through disengagement. The literature speaks of patients needing to finalize their lives. TR helped this patient achieve life closure with dignity and with her self identity intact.
According to the literature, cancer patients face depression throughout the course of their illness. TR provided a way for the patient to put her “sadness” on hold. She never used the word depressed but she exhibited sadness from time to time. The patient was able to focus on many activities that gave her the opportunity to set depressive emotions aside. She quietly grieved for patients she had met during TR who died before her. Regardless, in TR, she continued to establish new relationships with other patients and actively engaged in social interaction. This appears to have helped her emotional functioning given that TR provided her with opportunities to express her emotions in a socially appropriate way.
Loneliness is another consequence of the disease that has been addressed by the literature and is reduced by TR. The psycho-social supports provided by individual and group intervention reduces the stresses associated with dying. The patient’s involvement in TR provided a means to achieve palliation where, by virtue of being involved in TR programs, she was able to compare herself to other patients and realize that she was not alone in her situation.
Boredom is also a psycho-social symptom of the disease (Murphy, Morris & Lange, 1997). The patient was able to reduce boredom through TR using the acquisition of new leisure skills such as ceramics and horticulture. Although the patient struggled with certain projects that required a level of fine motor coordination, she was able to“ work” on these projects and over time finished everything she started. This gave her a sense of purpose and meaning which the authors Taylor (1992) and Stensrud (1993) both cite as being very important for palliation.
Cultural enrichment through group interaction occurs in TR. This enhances and promotes palliation for this patient. She became friendly with a number of other patients from culturally diverse populations. She demonstrated interest in learning about other cultures. The patient found this to be an opportunity to become involved with others. Whether being outside on the terrace or in a TR group on the unit, she was “involved” which allowed her to be distracted from her own demise. This effectively alleviates or reduces the anxiety associated with her own illness. For the patient, this helped her regain self esteem. Interactions in TR let the patient give and receive emotional and psycho-social support.
The patient’s independence was improved in part due to TR. Through TR the patient began to engage in self directed leisure activity, often with peers. The patient was admitted on oxygen and needed to be wheeled everywhere. In TR she literally stood up and found her feet again. She eventually convinced her doctor that she should be allowed to walk to the day room independently for recreation. Eventually she went on her own even when no formal program was being run. This would later (about 8 weeks post admission) lead to her engaging in her own leisure activities, unsupervised, in the evenings while all other patients were sleeping.
She needed contact, to be able to touch others, to voice concerns openly, which was difficult at times because her tracheotomy. She communicated by placing her right index finger over the opening, and whispered in a barely audible voice. Then she would reach out and touch.
TR helped the patient deal with loss. The adjustment to cancer always involves loss and impending loss. TR enabled the patient’s ego-coping mechanisms. It promoted her self esteem, gave her control, and helped her deal with obsessive compulsive behaviors such as smoking where she could engage in TR and wait for another cigarette.
The loss of control is another symptom that has been addressed here by TR. The patient was able to complete several projects, maintain peer relationships, and confront uncertainty through the support system provided by TR. This seems to support the findings of Aaronsen & Beckman, (1987) that the dying need rewarding and continued social interaction to reduce uncertainty, anxiety, and fear.
Negative feelings are also addressed and this seems to support Nuelinger’s personal community in leisure theory (Neulinger, 1981). The TR group provided a personal therapeutic community where the patient was able to confront the fear of death and other negative feelings. She was able to redirect and focus on what she was still able to accomplish.
Research by Rando (1981) indicated that the dying patient feels a need to accomplish something daily, even a small task. The patient here demonstrated this on several occasions and often took days to complete a task, a little bit each day. This has a palliative benefit in that the patient feels better having accomplished something.
The Calvary Hospital Assessment was conducted within 72 hours of admission and was used as an initial assessment of the patient. The fact that while communicating she had to whisper while covering her tracheotomy with her fingers was not mentioned on the assessment. This is because this information was found elsewhere in the chart and it is hospital policy not to duplicate information. The FACTR assessment was also used to conduct the study in an effort to gather additional information related to the patient’s level of functioning.
Therapeutic recreation professionals face a difficult challenge when working with patients who are at the end stage of life. The common denominator may be terminal illness for any given patient, but the challenge is addressing all of the various needs that the dying patient has. Often, upon first approach the therapist is told by the patient or a family member that there is no “need for recreation”. The response must always be one of hope. The therapist must educate the patient about the importance of social interaction. Explaining the palliative benefits of TR is an important aspect to establishing a therapeutic relationship with the patient. This does not mean that the therapist must start quoting the various theories discussed in the literature but, rather, the actual programs and opportunities available to the patient. The therapist must also state that he or she will return on a regular basis. This builds rapport and promotes interest in TR.
The patient’s biggest need was, perhaps, the need to have a dignified death. This was addressed by TR through her social interactions and a continuance of care. Once a relationship was established between the therapist and the dying patient, the therapist continued to monitor, assess, and provide TR interventions as appropriate.
Therapeutic recreation as part of the palliative approach to
treatment is a necessary practice and an important part of the
care a patient receives. The patient gets an improved quality of
life while receiving the palliative benefits of psycho-social
supports.
IMPLICATIONS & RECOMMENDATIONS
One implication of this study is that therapeutic
recreation can contribute to palliation by providing the dying patient with an opportunity to maintain his or her quality of life. Palliation through therapeutic recreation appears to help the dying patient live life to the fullest at the end stage of terminal illness. This study demonstrates how therapeutic recreation provides opportunities for a dying patient to socialize, maintain a sense of self, express creativity and learn new skills which lead toward life satisfaction despite the reality of impending death. This indicates that TR contributes to palliation to some degree.
There is very little on the relationship between palliation and therapeutic recreation in the TR literature. Further research on therapeutic recreation and palliation could be done. Perhaps a study of using single subject research design could be developed to further explore the relationship between palliation and therapeutic recreation. More data in this regard is needed and more studies could illustrate the importance of palliation for the individual patient at the end stage of the disease process.
The concept of palliation could also be applied to other populations and settings being served by therapeutic recreation. The idea would be to begin the palliative approach when the patient first attends a recreation therapy session. Practical recommendations include expanding palliative therapeutic recreation for patients with all types of illnesses or disabling conditions. In summary, therapeutic recreation has the potential to become a palliative treatment of all individuals in all clinical and community therapeutic recreation settings. Indeed, palliation as a treatment concept, could enhance the fundamental practice of service delivery.
REFERENCES
Aaronson, N.K. & Beckman, J.H. (1987) The quality of life of cancer patients, New York: Raven Press.
Bost, L. S. & Brown, E. M. (1982) Recreation therapy: A humanistic adjunct to oncology treatment. Oncology Nursing Forum , 9(4) 43-49.
Breitbart, W. & Holland, J. C. (1993) Psychiatric aspects of symptom management in cancer patients, Washington DC: The American Psychiatric Press.
Burlingame, J. & Blaschko, T. M. (1994) Assessment Tools For Recreation Therapy: Redbook #1. Revensdale, Washington. Idyll Arbor, Inc.
Cable News Online Network (1997), Cancer: Frequently Asked Questions, Atlanta Georgia.
Cimino, J. E. (1997) Commentary: Non-abandonment, physicians and nurses as allies, New York, The American Journal of Hospice & Palliative Care 14 (3) 106-107.
Connolly, P. (1993) Balancing changing health care needs with the shortage of quality health care professionals: Implications for therapeutic recreation, In M. P. Lahey , R. Kunstler, A. H. Grossman, F. Daly, S. Waldman & F. Schwarz (Eds.), Loss, Grief & Care, 6(4) . 15-21: NY: Haworth Press, Inc.
Davison, D. C. & Neale, J.M. (1996) Abnormal Psychology, New York: John Wiley & Sons Inc.
Harpham, W.S. (1994) After cancer: A guide to your new life, New York: W.W. Norton & Company.
Henderson, K. A.(1991) Dimensions of Choice, State College, PA: Venture Publications
Kavanaugh, R. E. (1972) Facing death, Baltimore, Maryland: Penguin Press.
Korchin, S. J. Modern Clinical Psychology (1976). New York: Basic Books.
Kubler-Ross, E. (1969) On death & dying, New York: Macmillan Publishing,
Lahey, M.P. (1993) Acute care vs. chronic care models of services to the elderly: Implications for therapeutic recreation, In M. P. Lahey , R. Kunstler, A. H. Grossman, F. Daly, S. Waldman & F. Schwarz (Eds.), Loss, Grief & Care, 6(4) . 55-62, New York: Haworth Press, Inc.
Lerner, M.(1994) Hedging the bet against cancer, New York: New York Times magazine.
Lowery, B.J. Jacobsen BS. & Ducette J.. (1993). Causal attribution, control, and adjustment to breast cancer. Journal of Psychosocial Oncology, 10(4) 41.
Malone M. & Harris A.L. (1993). Assessment of the impact of cancer on work, recreation, home management and sleep using a general health measure. Journal of Social Medicine, 87(7) 386
McDowell, I. & Newell, C. (1996) Measuring Health: A guide to rating scales & questionnaires, New York: Oxford University Press.
Muschel, I. J. (1984) Pet therapy with terminal cancer patients: The Journal of Contemporary Social Work, 62(10) 451-453.
Neulinger, J. (1981) The psychology of leisure: New York, Beacon Press.
OncoLink (1997) National Cancer institute fact sheet: Understanding prognosis and cancer statistics, Pennsylvania: University of Pennsylvania Cancer Center Online.
Rando, T. A. (1984) Grief, Death, & Dying: Clinical interventions for caregivers, Champaign: The Research Press. 227-250.
Steuer, F.B. (1994) The Psychological Development of Children. Pacific Grove, California. Brooks/Cole Publishing.
Stjernsward, J. & Colleau. S. M.(1996) The W.H.O. cancer pain and palliative care program: Past, present, and future, New York, Journal of Pain and Symptom Management, 12(2)), 65-66.
Stensrud, C. (1993) Quality of living until death: A fusion of death awareness into therapeutic recreation-leisure education, Loss, Grief, & Care, New York: 6(4) 33-37.
Stoll, B. A. (1988) Coping with cancer stress, The Netherlands: Nijhoff Publishers.
Taylor, E. J. (1992). The search for meaning among persons living with recurrent cancer. University of Pennsylvania. Ph.D. thesis.
Turk , D.C. & Feldman C. S. (1992) Noninvasive approaches to pain control in terminal illness: The contribution of psychological variables, The Hospice Journal, 8(1, 2) 31
Willetts, H. C. & Sperling, A. (1983) The role of therapeutic recreationist in assisting the oncology patient to cope, New York, Futura Publications.
